This spring, Lviv hosted the sixth Face to Face mission — a surgical program of the American Academy of Facial Plastic and Reconstructive Surgery (AAFPRS), implemented by Razom as part of the Co-Pilot project.
Over the course of seven days, a team of seven surgeons — Parag Gandhi, Grigoriy Mashkevich, Augustine Moscatello, John Frodel, Ryan Daniel Winters, Ivanna Nebor, Boris Chernobilsky — alongside ten nurses, including Susan Ketigian, Viktoriya Ygreen, Yurij Tsuvanyk, Jamie Harold Orange, Emmett Joseph Harty Jr, Maribel Caraballo, Andrew Kostyaniuk and Tashina Morgenstern, worked at the Military Medical Clinical Center of the Western Region together with their Ukrainian colleagues. They operated on patients with some of the most complex facial injuries caused by the war.
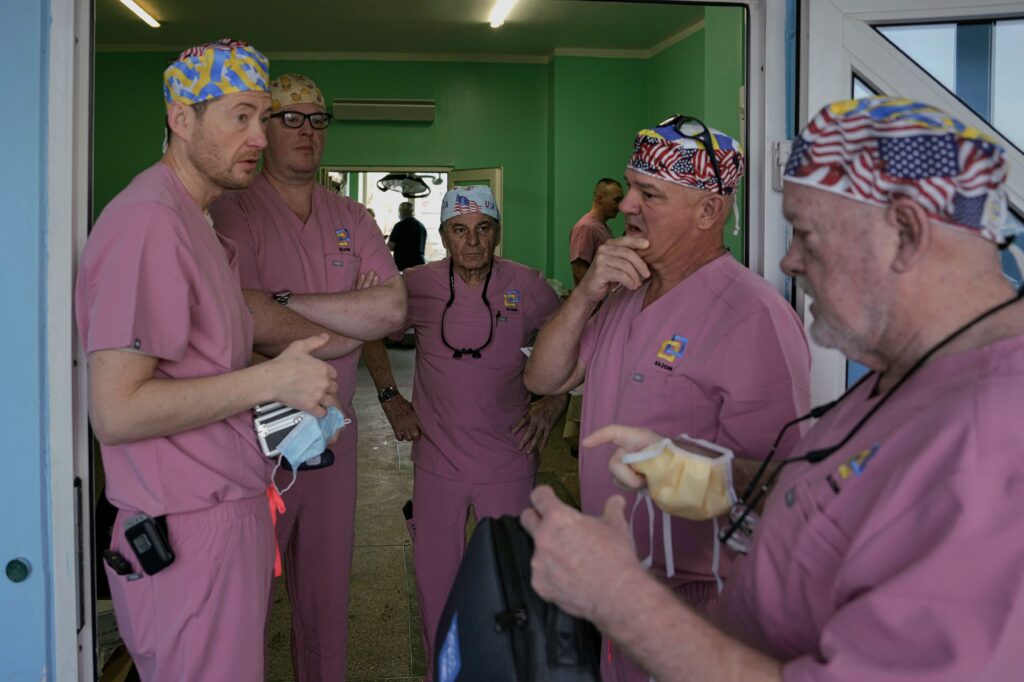

The work began with consultations: in just one day, doctors examined 55 patients and selected 40 for surgery. Starting the next morning, operating rooms ran at full capacity from 7 a.m. to 8 p.m. For four consecutive days, the team carried out reconstructive procedures across three specialties — ophthalmology, otolaryngology, and maxillofacial surgery. These injuries affect not only physical function but also how patients see themselves — their identity, confidence, and place in the world.
Among the patients were both military personnel and civilians affected by the war. For many, this was not the first stage of treatment, but part of a long recovery process that can last months or even years.
One of the defining features of this mission was the integration of surgical care with on-site prosthetics. Two anaplastologists — Eduardo Arias and Benjamin Rosenberg, specialists in ocular and facial prosthetics — joined the team. Together, they set up a temporary laboratory to create custom ocular prostheses for patients undergoing surgery.
This approach fundamentally changed the care pathway: patients were able to receive their prosthesis immediately after surgery, without waiting for a separate stage of treatment. In cases of eye loss, this has not only medical but also profound psychological significance — allowing individuals to return more quickly to a familiar appearance and to social life.

Alongside surgical care, the team also addressed other dimensions of recovery. Pain management specialist Timothy Canty, who works with PTSD, joined the mission. He delivered lectures at the Superhumans Center, Lviv Psychiatric Hospital, and St. Panteleimon Hospital, as well as practical trainings for anesthesiologists, psychologists, and pain management specialists at the Lviv Military Hospital. This work is aimed not only at supporting patients but also at strengthening the capacity of Ukrainian medical teams to address the long-term consequences of trauma.
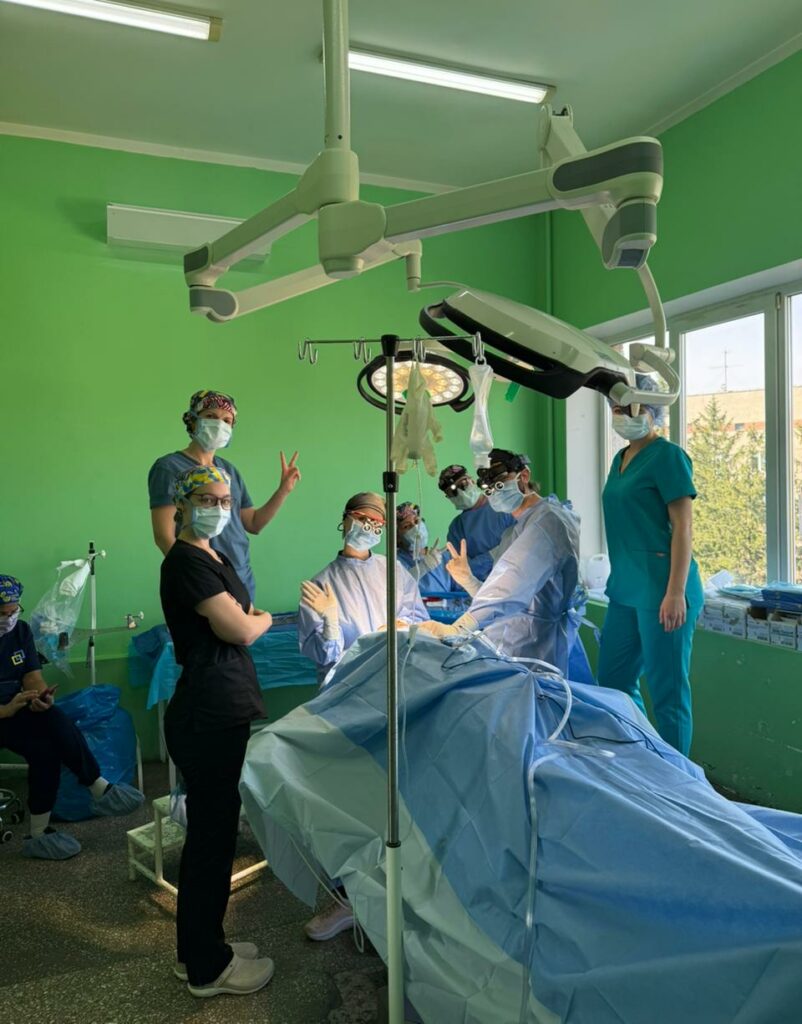
Knowledge transfer was another key component of the mission. Ukrainian doctors who had previously participated in missions, surgical trainings, conferences, and observerships in U.S. hospitals organized by Razom — as well as specialists from other Lviv hospitals — joined the procedures. They worked side by side with the international team in operating rooms, observing, assisting, and gaining experience they will continue to apply in their practice.

Dr. Parag Gandhi, an oculofacial plastic surgeon with more than 20 years of experience and a third-time participant in the mission, emphasized the importance of this collaboration:
“It is a great honor for me to work alongside Ukrainian colleagues, helping injured soldiers and civilians who have sacrificed so much for their families and their country. I truly believe that while one person cannot do everything, everyone can do something. And it is through knowledge exchange and collaboration that we make that contribution.”

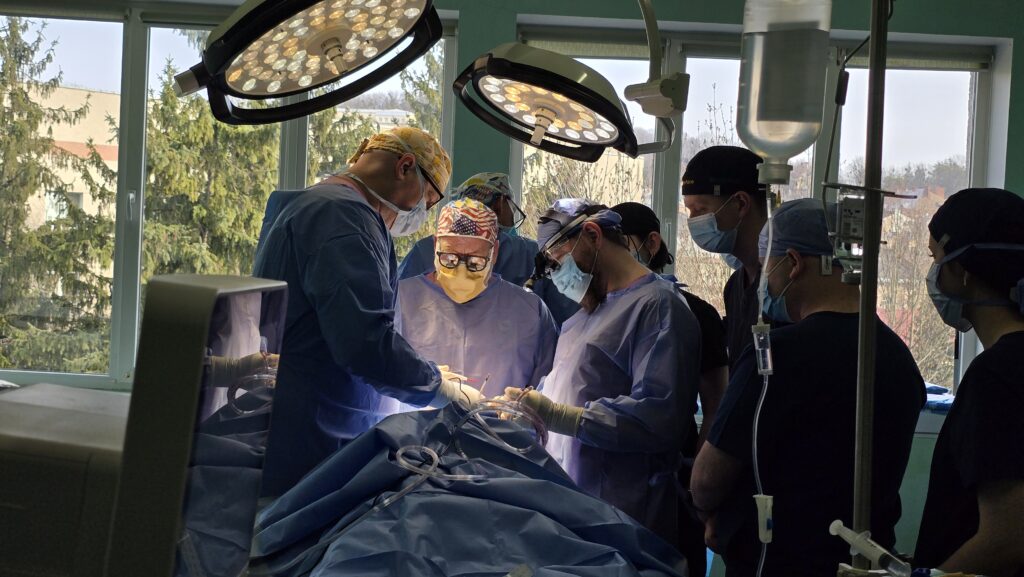
The mission was made possible through the partnership between Razom for Ukraine and the AAFPRS Face to Face program, as well as collaboration with the Military Medical Clinical Center of the Western Region, the INgenius platform, and Healing the Children North East.

These missions are gradually reshaping the approach to treating complex facial injuries in Ukraine. It is not only about individual surgeries, but about building a comprehensive model in which surgery, prosthetics, pain management, and physician training are integrated into a single, continuous process of recovery.
The mission was made possible by the support of Razom for Ukraine’s donors, whose contributions enable the deployment of international medical teams, procurement of critical equipment, and on-the-ground coordination. This support makes it possible not only to carry out complex surgeries, but also to facilitate the exchange of expertise between Ukrainian and international physicians and expand access to advanced approaches in treating war-related injuries.


