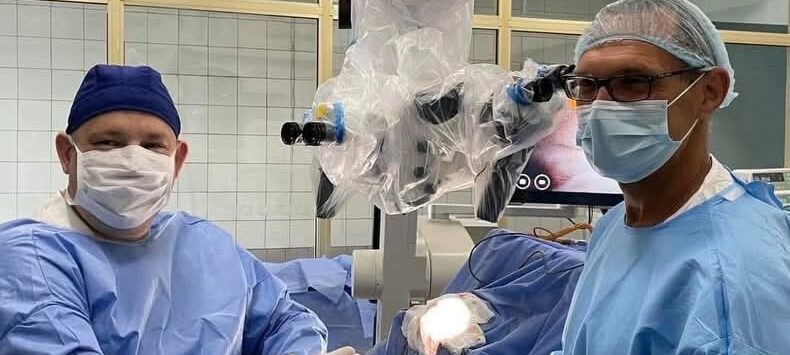
Ukrainian medicine under full-scale war is not only adapting. It is advancing how complex trauma care is delivered in active combat conditions.
Dnipro is a major city in eastern Ukraine, located along the Dnipro River and serving as a key medical hub for patients evacuated from front-line regions. Its hospitals receive a continuous flow of severely wounded patients from active combat zones.
Razom supports Mechnikov Hospital and the development of Co-Pilot to ensure Ukrainian medical professionals have access to modern tools, knowledge, and technologies needed to work under wartime conditions. This is support for a healthcare system that continues to save lives while strengthening the future of Ukrainian medicine.

In this system, the line between battlefield and hospital no longer exists. It runs through emergency departments, operating rooms, and daily clinical decisions. At Mechnikov Hospital, one of Ukraine’s leading referral centers for complex trauma, doctors are not only treating patients. They are building a model of care shaped by constant pressure, limited time, and high-risk injuries.
“We are now in Dnipro. This is my fourth trip here,” says American neurosurgeon Rocco Armonda. “We operate alongside Ukrainian doctors, manage intensive care, consult on complex cases, and work on scientific publications.”
This is not a typical professional exchange. It is sustained collaboration built around real-time needs. Razom supports this work by connecting specialists, helping with the logistics, delivering critical equipment, and enabling continuous knowledge exchange between Ukrainian and international doctors.
“Rocco was the first neurosurgeon who came to Dnipro in 2023,” says Andrii Sirko, head of neurosurgery at Mechnikov Hospital. “Since then, we have worked together every year, including on the most complex cases.”
This partnership reflects a broader shift. Wartime medical practice in Ukraine is contributing to new clinical standards that are now being observed internationally.
The First Trip: Suitcases, a Train, and the Unknown
Rocco’s first trip to Ukraine was defined by logistics and uncertainty.
“We flew to Kraków with four large containers of medical equipment,” Armonda recalls. “The vehicle we received was too small. We had to repack everything by hand.”
From there, the route continued to Lviv, across the border, and onward by overnight train to Dnipro. In Dnipro, the arrival was direct and personal.
“I was surprised. Senior doctors were waiting for us at the platform. That does not happen in the United States,” he says. Sirko remembers the same moment differently. “We first saw the suitcases. Only then we saw Rocco.”
This reflects the nature of the work. Action comes first.



The Operation That Changes the Understanding of War
The first day in the hospital required immediate engagement.
“It was a penetrating brain injury after a drone strike,” says Armonda. The injury involved both brain tissue and major vessels. Cases like this require rapid, multi-stage intervention. At Mechnikov Hospital, the team completed diagnosis and surgery without delay.
“I have not seen this done in one stage so close to an active combat zone,” Armonda notes. “In Iraq and Afghanistan, we focused on stabilization only.”
Ukrainian teams operate differently. They manage full clinical complexity under pressure. In another case, a patient presented with a gunshot wound to the base of the skull and intracerebral hematoma.
“I asked if observation was the plan,” Armonda recalls. Sirko’s response was direct. “No. We intervene.”
This approach prioritizes outcome and responsibility for survival. During the same period, the team introduced a pupillometer, a device used to assess neurological response and intracranial pressure. The equipment was delivered through international support and immediately integrated into clinical practice. The patient survived. This outcome reflects a consistent system, not an isolated case.

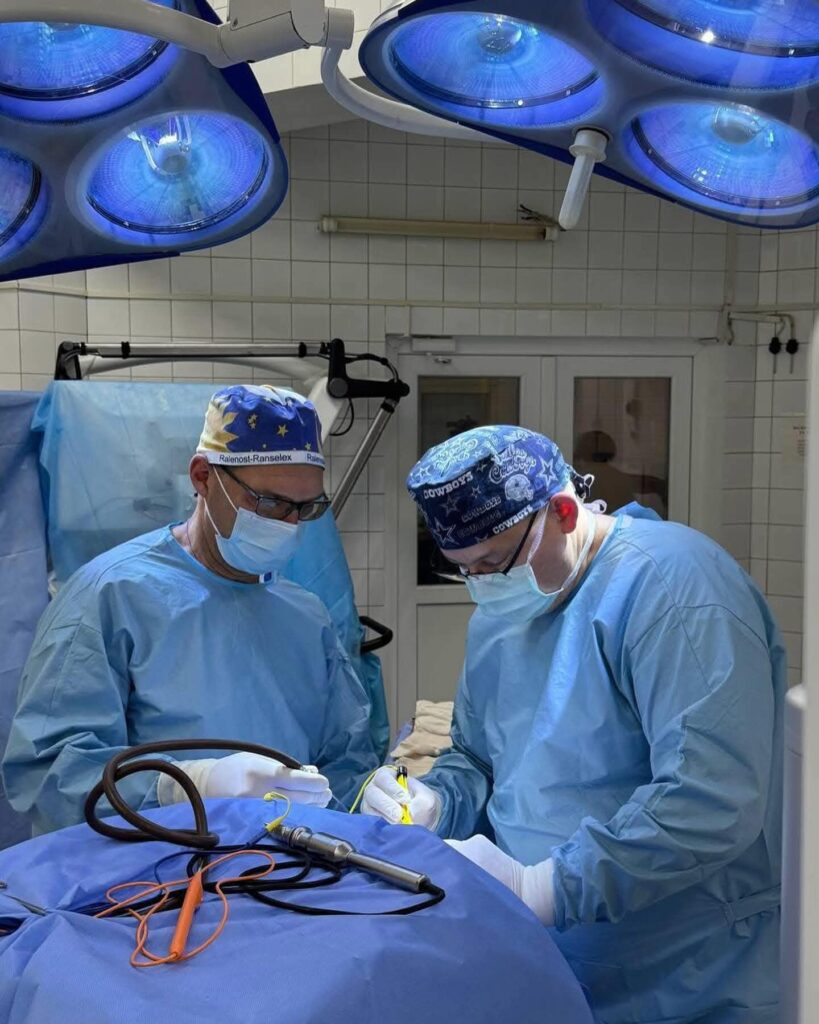
Philosophy of Survival and Work
War compresses time and changes decision-making.
“In the United States, we may observe for several days,” says Armonda. “Here, decisions must be immediate. The patient flow does not stop.”
Evacuation delays also affect treatment.
“Patients often arrive later than expected. This changes surgical planning, especially in the presence of infection. ”Adaptability defines the system. Ukrainian doctors adjust protocols in real time based on conditions on the ground. What stands out is not only clinical capability, but professional mindset. “People focus on what needs to be done today,” Armonda says.
“They go to work, treat patients, take care of their families.” Recognition is secondary. “When you call them heroes, they say they are doing their job. They point to those at the front.”
This reflects a clear professional ethic grounded in responsibility.
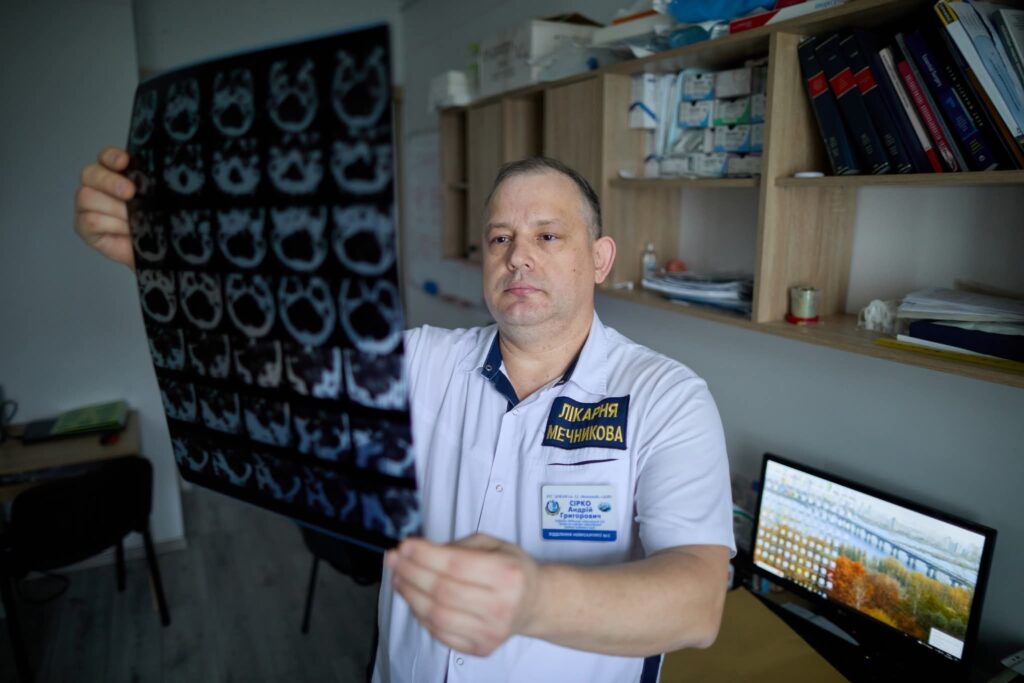
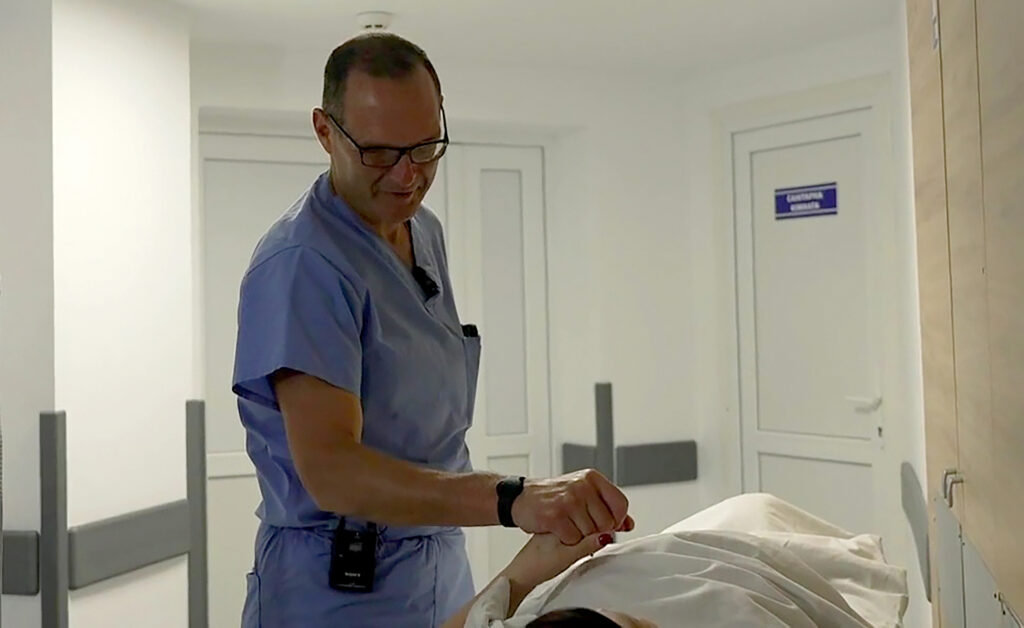
Why Advocacy Is a Continuation of Medicine
The discussion then moves beyond clinical work.
“People often ask me how they can help,” says Armonda.
“They contribute equipment, research, and funding. This supports patient care in a direct way.”
Every contribution is applied in practice, whether through equipment, medical missions, or research. In operational terms, this acts as a force multiplier. Support increases the capacity to treat more patients and manage more complex cases.
This is not only financial support. It is presence. People understand that they are not working in isolation. Razom maintains active operations in Ukraine, ensuring that support reaches hospitals where it is needed. This support is visible. It directly contributes to patient survival.
“We provide a platform so that the world can see what is happening here,” Armonda says. “People want to help.”
“We do not just work together. We begin to think in the same way,” adds Sirko.
“This matters beyond medicine. We share principles and apply them in daily work.” This includes not only treatment, but also sharing experience and making it visible to others. Without this exchange, the connection between teams would not exist. This work includes doctors, partners, and supporters across countries. It is coordinated and sustained.

From Practice to Advocacy
In this context, advocacy is not based on statements. It is based on demonstrated capability. It does not begin in political offices. It is formed in hospitals, through clinical decisions and responsibility for patient outcomes. Doctors do not describe this work as advocacy. They operate, train, and share clinical experience. By doing so, they provide direct evidence of what is possible in wartime medicine. In modern war, outcomes matter. The ability to make decisions, manage complexity, and save lives under pressure builds trust and informs international understanding. Ukraine’s experience is not only about survival. It contributes to the development of medical practice. As this experience becomes visible through research, collaboration, and exchange, it becomes part of the global medical conversation. Advocacy ensures that this work is understood. Because their experience is not a position. It is evidence.